As a health professional, I’ve witnessed firsthand the devastating toll drug abuse can take, not just on an individual’s life, but on their very essence – their brain. Understanding how drugs affect the brain is not merely an academic exercise; it’s a critical step in effective drug abuse recovery education. This comprehensive article aims to demystify the complex interplay between substances and our most vital organ, providing crucial insights for those seeking knowledge, support, or a path to recovery.
The Brain: Our Command Center and the Target of Addiction
To comprehend the impact of drugs, we must first appreciate the brain’s incredible complexity. It’s the command center for everything we think, feel, and do. Billions of neurons communicate through intricate networks, using chemical messengers called neurotransmitters to relay information. This delicate balance governs our mood, memory, learning, motivation, and reward systems – all of which become targets in the insidious grip of drug abuse.
Our brains are hardwired for survival and pleasure. Activities like eating, social connection, and achieving goals naturally stimulate the release of dopamine, a neurotransmitter associated with pleasure and reward. This “feel-good” sensation reinforces healthy behaviors, encouraging us to repeat them. This innate reward pathway, however, is precisely what drugs hijack.
The Hijacking of the Reward System: A Deeper Dive

Imagine a finely tuned orchestra. Each section plays its part, contributing to a harmonious melody. Now, imagine a powerful amplifier suddenly connected to just one instrument, drowning out all others and creating a deafening, distorted sound. This analogy begins to scratch the surface of how drugs hijack the brain’s reward system.
When drugs enter the brain, they often trigger an exaggerated surge of dopamine, far beyond what natural rewards can produce. For instance:
- Stimulants (e.g., cocaine, methamphetamine): These drugs block the reuptake of dopamine, leading to an accumulation in the synaptic cleft – the space between neurons. This prolonged and intense dopamine signaling creates euphoria, increased energy, and heightened alertness.
- Opioids (e.g., heroin, oxycodone): Opioids mimic natural endorphins, binding to opioid receptors and releasing a flood of dopamine. This produces intense feelings of pleasure, pain relief, and relaxation.
- Cannabis (e.g., marijuana): THC, the active compound in cannabis, binds to cannabinoid receptors, which are involved in regulating mood, memory, and appetite. While the exact mechanism is complex, it also influences dopamine release, contributing to the characteristic “high.”
- Alcohol: Alcohol has a more global effect, interacting with multiple neurotransmitter systems, including GABA (an inhibitory neurotransmitter) and glutamate (an excitatory neurotransmitter), while also increasing dopamine.
This artificial overstimulation of the reward pathway creates a powerful, often irresistible drive to repeat drug use. The brain starts to re-prioritize drug-seeking behavior above all else, diminishing the appeal of natural rewards.
Neuroadaptation: The Brain’s Attempts to Cope
The brain is remarkably adaptable. In response to the chronic overstimulation caused by drug abuse, it attempts to restore balance through a process called neuroadaptation. This involves several changes:
- Downregulation of Receptors: The brain may reduce the number of dopamine receptors or make them less sensitive. This means that more of the drug is needed to achieve the same pleasurable effect, a phenomenon known as tolerance.
- Changes in Neurotransmitter Production: The brain may also reduce its own natural production of dopamine and other neurotransmitters. This is why, when drug use stops, individuals often experience anhedonia – the inability to feel pleasure from normal activities – and profound depression.
- Alterations in Stress Pathways: Chronic drug use also impacts the brain’s stress response system. The amygdala, involved in fear and anxiety, becomes hyperactive, contributing to intense cravings and withdrawal symptoms.
These neuroadaptations are crucial to understanding the vicious cycle of addiction. The brain becomes accustomed to the presence of the drug, and its absence triggers significant discomfort, both physical and psychological.
The Impact on Cognitive Functions: Beyond Pleasure

The effects of drugs extend far beyond the reward system. They significantly impair critical cognitive functions, impacting an individual’s ability to think, learn, and make decisions.
- Memory: Drugs can interfere with the hippocampus, a brain region vital for memory formation and retrieval. This can lead to difficulties recalling recent events, learning new information, and even remembering important aspects of their lives.
- Learning: The ability to learn from experience and adapt behavior is compromised. This makes it challenging for individuals in active addiction to learn from past mistakes or to acquire new coping mechanisms.
- Decision-Making and Impulse Control: The prefrontal cortex, responsible for executive functions like planning, judgment, and impulse control, is significantly affected. This leads to impaired decision-making, increased impulsivity, and a reduced ability to resist drug cravings, even when aware of the negative consequences.
- Emotional Regulation: The intricate balance of emotions is disrupted. Individuals may experience heightened irritability, anxiety, mood swings, and an inability to manage stress effectively without the drug.
These cognitive deficits contribute to the destructive behaviors associated with addiction, making it incredibly difficult for individuals to escape the cycle without comprehensive support and drug abuse recovery education.
Long-Term Neurological Consequences: A Lasting Imprint
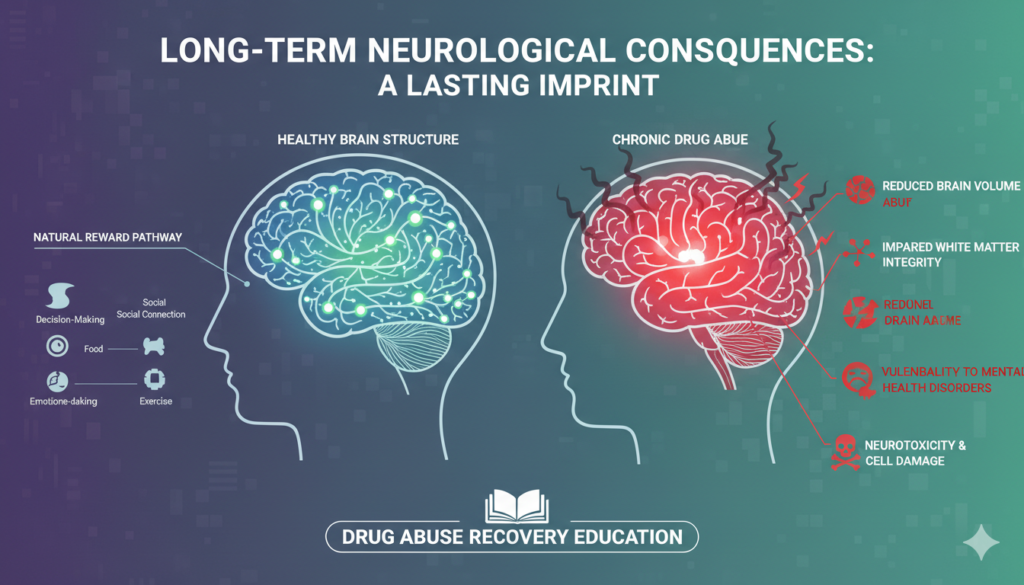
The repeated exposure to drugs can lead to long-lasting structural and functional changes in the brain. While some degree of recovery is possible with abstinence, certain effects can persist for extended periods or even be permanent.
- Reduced Brain Volume: Studies have shown that chronic drug abuse can lead to a reduction in gray matter volume in various brain regions, including the prefrontal cortex, which is critical for higher-level thinking.
- Impaired White Matter Integrity: White matter, composed of myelinated nerve fibers, facilitates communication between different brain regions. Damage to white matter can disrupt these crucial connections, leading to slower processing speeds and cognitive difficulties.
- Increased Vulnerability to Mental Health Disorders: Drug abuse is frequently co-occurring with mental health conditions such as depression, anxiety disorders, and psychosis. This is a complex relationship, as drugs can exacerbate existing vulnerabilities or even trigger the onset of these conditions.
- Neurotoxicity: Some drugs, particularly methamphetamine and ecstasy, can be directly neurotoxic, causing damage to dopamine and serotonin-producing neurons. This can have profound and lasting impacts on mood, memory, and cognitive function.
Understanding these long-term consequences underscores the urgency and importance of early intervention and effective drug abuse recovery education.
The Role of Genetics and Environment: A Complex Web
While drugs directly impact the brain, it’s crucial to acknowledge that individual vulnerability to addiction is influenced by a complex interplay of genetic and environmental factors.
- Genetic Predisposition: Research indicates that genetics can account for approximately 40-60% of an individual’s risk for developing a substance use disorder. Certain genes may influence how a person metabolizes drugs, their brain’s reward response, or their predisposition to impulsivity and risk-taking.
- Environmental Factors: Early childhood trauma, stress, peer pressure, lack of parental supervision, socioeconomic status, and easy access to drugs all contribute to environmental risk factors.
- Comorbidity with Mental Health Disorders: As mentioned, co-occurring mental health conditions significantly increase the risk of addiction. Individuals may self-medicate uncomfortable symptoms of anxiety or depression with drugs, creating a dangerous feedback loop.
This holistic perspective is vital for effective drug abuse recovery education, as it informs tailored treatment approaches that address not only the neurological aspects of addiction but also the underlying psychological and social vulnerabilities.
The Brain in Recovery: Healing and Rebuilding
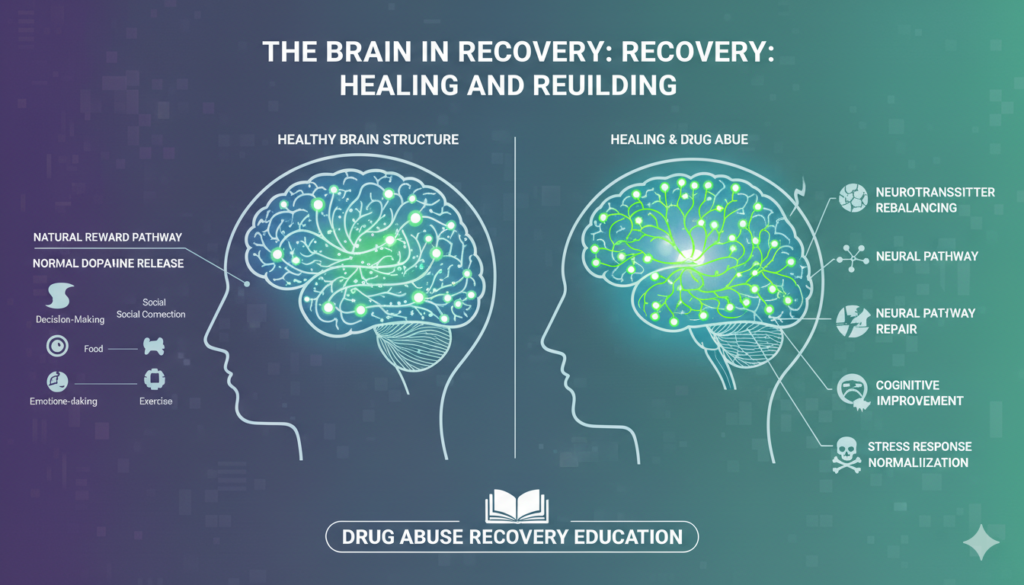
The good news is that the brain possesses remarkable plasticity, its ability to change and adapt. While recovery is a challenging journey, the brain can begin to heal and rewire itself with sustained abstinence and appropriate support.
- Neurotransmitter Rebalancing: Over time, with abstinence, the brain can gradually begin to restore its natural production of dopamine and other neurotransmitters, and receptor sensitivity can improve. This leads to a gradual return of the ability to experience pleasure from natural rewards.
- Neural Pathway Repair: New neural pathways can form, strengthening connections in areas of the brain responsible for healthy decision-making, emotional regulation, and impulse control.
- Cognitive Improvement: As the brain heals, cognitive functions like memory, attention, and executive function can improve significantly. This empowers individuals to engage more effectively in therapy, learn new coping skills, and rebuild their lives.
- Stress Response Normalization: The hyperactive stress response system can gradually calm down, leading to reduced anxiety and improved emotional regulation.
This healing process is not linear and requires sustained effort, but the brain’s capacity for recovery offers immense hope for those struggling with addiction.
Drug Abuse Recovery Education: The Cornerstone of Healing
Understanding how drugs affect the brain is not just theoretical; it’s the bedrock of effective drug abuse recovery education. This knowledge empowers individuals in several ways:
- Demystifying Addiction: It helps people understand that addiction is a chronic brain disease, not a moral failing. This reduces stigma and encourages individuals to seek help without shame.
- Motivating Treatment: When individuals understand the profound impact drugs have had on their brain, it can be a powerful motivator to commit to treatment and recovery.
- Explaining Withdrawal Symptoms: Knowledge of neuroadaptation helps explain the intense physical and psychological discomfort of withdrawal, preparing individuals for what to expect and reinforcing the need for medically supervised detoxification.
- Enhancing Relapse Prevention: Understanding the persistent cravings and triggers related to altered brain pathways equips individuals with strategies to manage these challenges and prevent relapse.
- Promoting Healthy Coping Mechanisms: Education about the brain’s natural reward system encourages the adoption of healthy coping mechanisms that stimulate dopamine naturally, such as exercise, mindfulness, hobbies, and social connection.
- Informing Loved Ones: Educating family and friends about the neurological basis of addiction helps them understand their loved one’s struggles, foster empathy, and provide more effective support.
Effective drug abuse recovery education should be integrated into every stage of the recovery process, from initial intervention and detoxification to long-term aftercare and relapse prevention.
Components of Comprehensive Drug Abuse Recovery Education
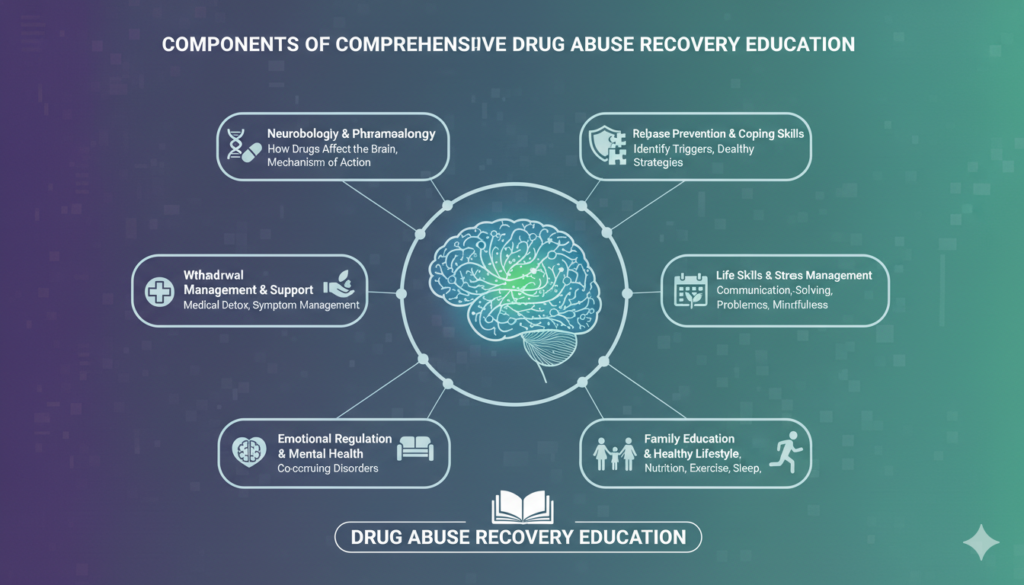
A robust drug abuse recovery education program encompasses various elements, tailored to individual needs:
- Neurobiology of Addiction: Detailed explanations of how specific drugs impact neurotransmitters, brain structures, and cognitive functions. This can be greatly enhanced with visual aids like infographics.
- Pharmacology of Drugs: Understanding the mechanisms of action, effects, and potential risks of different substances.
- Withdrawal Management: Education on the symptoms of withdrawal, the importance of medical supervision, and strategies for managing discomfort.
- Relapse Prevention Strategies: Teaching individuals to identify triggers, develop coping skills, and create a strong support system.
- Coping with Cravings: Techniques for managing intense cravings, including distraction, mindfulness, and seeking support.
- Life Skills Development: Rebuilding essential life skills that may have deteriorated during active addiction, such as communication, problem-solving, and financial management.
- Stress Management: Learning healthy ways to cope with stress, a common trigger for relapse.
- Emotional Regulation: Developing skills to understand and manage emotions without resorting to substance use.
- Healthy Lifestyle Choices: Emphasizing the importance of nutrition, exercise, sleep, and overall well-being in supporting brain recovery.
- Family Education: Providing resources and support for family members to understand addiction and learn how to best support their loved one’s recovery.
- Co-occurring Disorders: Addressing the complex interplay between addiction and mental health conditions, providing integrated treatment strategies.
The Power of Visuals: Infographics in Recovery Education
In today’s information-rich world, visuals play a critical role in conveying complex information effectively. This is where infographics shine, particularly in drug abuse recovery education. An infographic titled “How Drugs Affect the Brain” can simplify intricate neurological processes into easily digestible visual representations.
Imagine an infographic that clearly illustrates:
- The healthy reward pathway with natural dopamine release.
- How different drugs (e.g., cocaine, opioids) flood the brain with dopamine.
- The concept of tolerance and receptor downregulation.
- The impact on the prefrontal cortex and impaired decision-making.
- The long-term effects on brain structure.
- The healing process in recovery.
Such a visual tool can enhance understanding, improve retention of information, and make complex scientific concepts accessible to a wider audience, from individuals in recovery to their families and even policy-makers. It can be a powerful catalyst for initiating crucial conversations and fostering empathy.
Conclusion: A Path Towards Informed Recovery
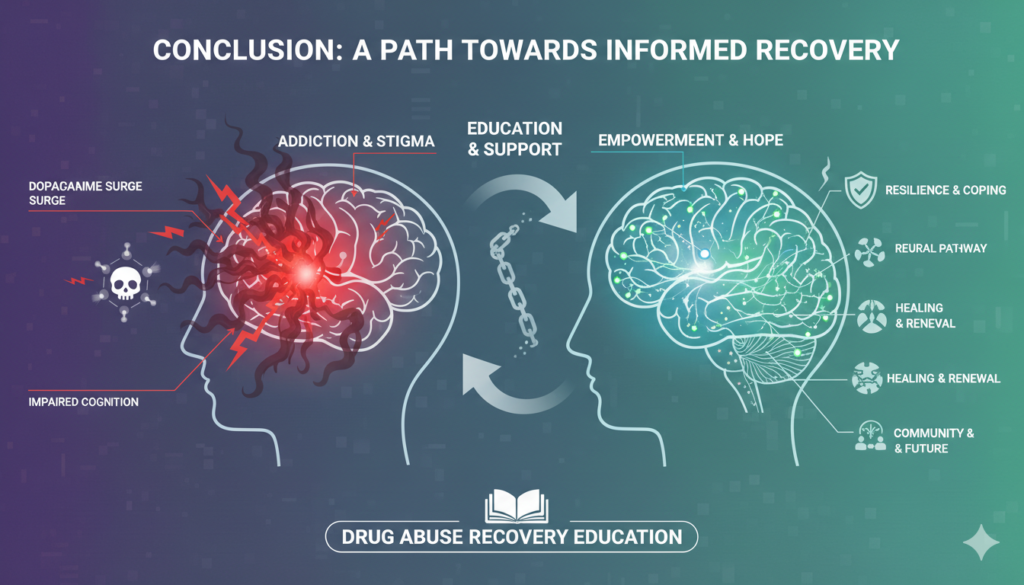
Understanding how drugs affect the brain is not just about scientific knowledge; it’s about empowering individuals, families, and communities with the tools for healing and hope. Addiction is a formidable challenge, but with comprehensive drug abuse recovery education rooted in scientific understanding, we can dismantle stigma, promote effective treatment, and pave the way for lasting recovery.
The brain, though resilient, bears the scars of addiction. Yet, it also holds the incredible capacity for repair and renewal. By embracing education, fostering empathy, and providing robust support systems, we can guide individuals on a journey of healing, helping them reclaim their minds, their lives, and their futures. The path to recovery begins with knowledge, and for those ready to embark on that journey, understanding the brain’s intricate dance with drugs is the first, most crucial step.




